(Def.) Notified bodies are “designated” by the EU member states (sometimes also referred to as “notifed”), usually private companies that assume sovereign tasks, including the “approval” and monitoring of medical devices.
Content
On this page, you will find articles on:
- Tasks and responsibilities of notified bodies
- Finding a notified body
- Influence of regulatory requirements on notified bodies
- FAQ on notified bodies
- Criticism of notified bodies
- Support in dealing with notified bodies
1. Tasks and responsibilities
Manufacturers must always involve notified bodies such as TÜVs if they wish to place a medical device on the market in the EU that does not fall into the lowest “risk class” (class I).
Depending on the conformity assessment procedure chosen by the manufacturer, the tasks of the notified bodies consist of
- examining the technical documentation or/and
- examining each individual device or/and
- examining a type or/and
- auditing, certifying, and monitoring a quality management system. This also includes unannounced audits.
However, the manufacturer remains responsible for the conformity of medical devices with legal requirements such as the Medical Device Regulation (MDR) and the national laws as for instance the Medical Device Implementation Act (MPDG) in Germany.
Caution!
Please note that many notified bodies contractually oblige manufacturers to report every product change. Whether the notified bodies then check this is another matter. The law does not stipulate that manufacturers may only continue to market their devices subject to the output of these inspections as long as manufacturers act within the scope of their certificate.
However, manufacturers must comply with Annex IX Paragraph 2.4 of the MDR in this context. According to it, manufacturers must inform their notified bodies of any significant changes to their devices and the QMS.
The Johner Institute helps to decide whether a significant change has occurred.
2. Finding notified bodies
An overview of notified bodies can be found on these pages:
- ZLG (German “Zentralstelle der Länder für Gesundheitsschutz bei Arzneimitteln und Medizinprodukten” – Central Office of the Federal States for Health Protection for medicinal products and medical devices)
- EU Commission: Notified bodies for the MDR (also outside Germany)
- Entry page for searching in specific countries or designations
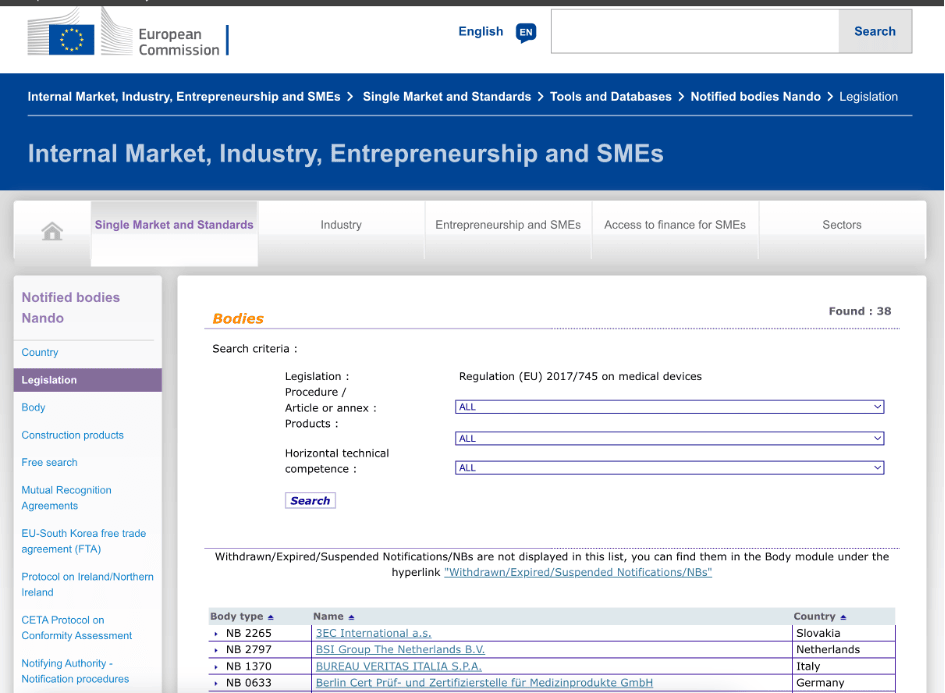
Fig. 1: Screenshot of the EU database (NANDO), where you can search for notified bodies for the MDR and IVDR.
3. Impact of regulatory changes
a) Conversion to the MDR/IVDR
All organizations must be (re)designated for the MDR and IVDR. The consequences are
- a defect and thus a bottleneck of notified bodies and
- long waiting times and rising prices.
b) Brexit
Brexit also affected notified bodies based in the UK. The EU published a statement on this, and the notified body BSI has taken a step forward: They operate from the Netherlands (press release).
4. FAQ on notified bodies
Question 1: Do you have any recommendations for notified bodies?
The Johner Institute works well with all notified bodies and is recommended by most notified bodies. Because not all notified bodies are equally suitable for all topics or product groups, we can only make a specific recommendation if you let us know more about your device and your company (contact form).
Question 2: Is there a difference in the notified bodies’ strictness level?
This question can now be answered in the negative. The differences between the auditors of a notified body are often greater than the differences between the notified bodies themselves.
Question 3: Do costs differ depending on which notified bodies are involved?
Yes, because notified bodies are not subject to price regulations like pharmacies, for example, even if the prices sometimes suggest this ;).
Tip
Get quotes and compare them. If you need help with the evaluation, let us know.
Question 4: When do I need a notified body?
You always need a notified body, except for class I devices. It may also be necessary for you to involve a test laboratory. Although notified bodies also operate test laboratories, not all test laboratories are MDR respectively IVDR notified bodies.
Question 5: How long does it take to find a notified body?
It isn’t easy to give a dependable answer. A distinction must be made between different periods:
- The time it takes for the notified bodies to respond to a request
- The duration of the application process that results in a contract
- The time that elapses before the notified body conducts an audit
- The time taken for the inspection of the technical documentation
- The time it takes for the notified bodies to issue the certificate
Note
There are notified bodies that do not respond to requests or only respond after a long time. However, they may also be available quickly, e.g., if an appointment with another customer has been canceled.
You should base your audit appointment on your planning and not primarily on the availability of a notified body. Read more about the time schedule here.
5. Criticism of notified bodies
The notified bodies have a balancing act to master:
On the one hand, they compete with each other and could be tempted to win over customers (medical device manufacturers) through generous controls.
On the other hand, they are also subject to inspections by the authorities and must ensure that no safety-critical devices are placed on the market.
Point of criticism 1: Insufficient capacity and response times
In the meantime, national authorities are intensively examining notified bodies, with the output that many notified bodies have withdrawn or lost their designation. As a result, the remaining notified bodies are overloaded. Accordingly, the speed of responding to inquiries, arranging appointments, and certifying quality management systems suffers.
Point of criticism 2: Exploding prices
The overload of notified bodies and the lack of competition sometimes lead to customer-unfriendly behavior and often to exploding prices.
Note
The digitalization of notified bodies makes it possible to increase both the efficiency and effectiveness of notified bodies substantially. The Johner Institute already supports notified bodies in their digital transformation.
Criticism 3: Inconsistent and unfounded requirements
There is much criticism of auditors and reviewers of technical documentation:
- Their requirements are not sufficiently homogeneous either within a notified body or between notified bodies.
- Many reviews and audits are limited to formal aspects. For example, reviewers of notified bodies write deviations if an expected word does not appear in a clinical investigation.
- They also impose requirements that cannot be justified either by the regulatory requirements (MDR, IVDR) or requirements stated in (harmonized) standards. Concerning the state of the art, they demand conformity with the requirements of the (sometimes questionable in terms of quality) MDCG guidelines, although these guidelines describe themselves as non-binding.
6. Support
Are you unsure how to get your medical device through the entire conformity assessment (“approval”) process quickly, safely, and without unnecessary costs? The Johner Institute team will be happy to help! Get in touch with us!
Contact us
